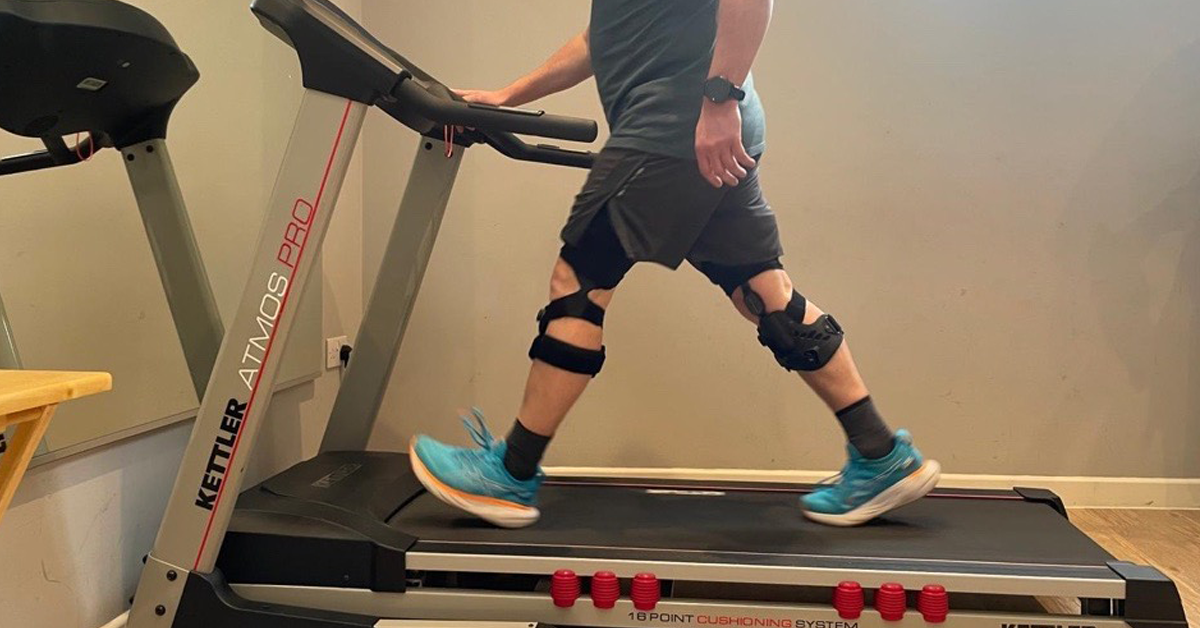
Anterior cruciate ligament (ACL) injuries are among the most significant musculoskeletal injuries encountered in clinical practice, affecting active individuals and athletes across a wide range of sports and activity levels. The immediate post-injury period has traditionally been viewed as a preparatory phase before surgical or non-surgical treatment begins. However, emerging evidence suggests that the decisions made in the first days and weeks after injury – including whether and how to brace the knee – may have a meaningful influence on both healing biology and joint stability.
This article examines two recent clinical studies that shed new light on early mechanical control as an active component of acute ACL management, with implications for clinicians across both non-surgical and surgical care pathways.
Why Early Mechanical Control Matters in Acute ACL Injury
Early management is a well‑established component of acute anterior cruciate ligament (ACL) injury care. Emerging evidence now places increased focus on the mechanical environment created in the immediate post‑injury phase, suggesting that early mechanical control of the knee may influence both biological healing processes and functional stability.
Recent clinical studies examining early bracing strategies highlight that temporary immobilization after ACL rupture may be associated with favorable outcomes through different but complementary mechanisms, supporting ligament healing pathways identifiable on MRI in selected patients, and reducing high‑grade rotational instability associated with injury to anterolateral knee structures. Together, these findings invite a closer examination of early bracing as an active component of acute ACL injury management rather than a purely interim measure.
MRI-Guided Healing Pathways: The Cross-Bracing Protocol
A prospective case series1 investigated outcomes in 80 consecutive patients who presented within 4 weeks of acute ACL rupture and were managed non‑surgically using the Cross‑Bracing Protocol (CBP). The protocol involved knee immobilization at 90° of flexion in a 4-point knee ligament brace with ROM control for 4 weeks, followed by progressive increases in range of motion until brace removal at 12 weeks, alongside physiotherapist‑supervised, goal‑oriented rehabilitation. MRI was performed at 3 and 6 months, with ACL healing graded using the ACL Osteoarthritis Score (ACLOAS).
At 3 months, 90% (72/80) of patients demonstrated MRI evidence of ACL continuity. Healing was graded as ACLOAS grade 1 (thickened or taut ligament) in 50%, grade 2 (thinned or elongated ligament) in 40%, and grade 3 (absent ligament or discontinuity) in 10% of patients. Patients with ACLOAS grade 1 reported higher Lysholm and ACL‑QOL scores, demonstrated lower passive knee laxity, and had higher rates of return to pre‑injury sport at 12 months compared with those graded ACLOAS 2–3. ACL re‑injury occurred in 14% of patients, primarily during high‑force or high‑velocity activities.
Refining Patient Selection: ACL-ARCH MRI Criteria
Building on experience managing over 1080 active individuals and athletes with CBP, a subsequent publication2 proposed the ACL Acute Rupture Characteristics for Healing (ACL‑ARCH) MRI criteria to better characterize acute ACL rupture severity in relation to potential non‑surgical healing. The authors describe four key MRI features relevant to healing potential: integrity of femoral and tibial attachment, displacement of ACL tissue outside the intercondylar notch, gap distance between torn ends, and retraction of ACL ends into rounded stumps (“involution”).
Within the first 80 patients treated with CBP, partial femoral avulsion and displacement of ACL tissue outside the intercondylar notch were more frequently observed in patients with thinned, elongated, or absent healing on 3‑month MRI. Larger gap distances (≥7 mm) were also more common in patients with poorer healing outcomes.
The authors recommend minimum 1.5T MRI (3T preferred) and the use of double‑oblique sequences to optimize visualization of ACL fibers when assessing these features.
Early Post-Traumatic Bracing and Rotational Knee Stability
A multicenter retrospective consecutive study3 examined 168 patients who underwent ACL reconstruction and compared outcomes between those who received early post‑traumatic knee immobilization and those who did not. Of the total cohort, 132 patients received a knee brace (hinged or non‑hinged), while 36 patients received no immobilization. The mean time from trauma to bracing was 0.8 days, and the mean duration of immobilization was 23.9 days. Patients were allowed full weight-bearing after immobilization.
The primary outcome was the severity of pivot shift, assessed intra‑operatively under general anesthesia. A grade 3 pivot shift was observed in 27% (44/168) of patients overall and was significantly more frequent in patients without a brace compared with those who received early bracing (50% vs 19.7%, p = 0.0012). Both hinged and non‑hinged braces were associated with a lower risk of grade 3 pivot shift, with odds ratios of 0.221 and 0.232, respectively. Immobilization lasting ≤3 weeks was associated with a higher risk of grade 3 pivot shift compared with immobilization for >3 weeks.
The authors conclude that early post-injury bracing was associated with a lower incidence of high-grade rotational instability before ACL reconstruction. They suggest that systematic immobilization after knee trauma could be advocated based on these findings.
Two Studies, One Shared Message
Although the two studies differ in design, patient populations, and primary outcomes, they converge on a shared principle: the early mechanical environment of the injured knee matters. The CBP and ACL-ARCH publications describe how early immobilization combined with MRI assessment can provide insight into ACL healing characteristics and rupture severity, while the multicenter surgical cohort study demonstrates that early bracing is associated with reduced high-grade rotational instability at the time of reconstruction. Together, these findings highlight early bracing as a potentially influential factor across different acute ACL care pathways.
Key Take-Home Messages
- Early mechanical control of the knee is a management variable in the acute phase after after ACL rupture
- Structured early bracing has been associated with:
- MRI‑observed ACL healing characteristics
- Reduced incidence of high‑grade pivot shift before ACL reconstruction
- Healing potential and rotational stability represent distinct but complementary outcomes
- Early bracing may be relevant across both non‑surgical and surgical ACL care pathways
Supporting ACL Care with DonJoy® Bracing Solutions
The evidence discussed in this article points to the importance of providing appropriate mechanical control at every stage of ACL injury management – from the immediate post-injury period through to return to sport. Enovis™ offers two DonJoy® bracing solutions designed to support clinicians across this continuum of care.
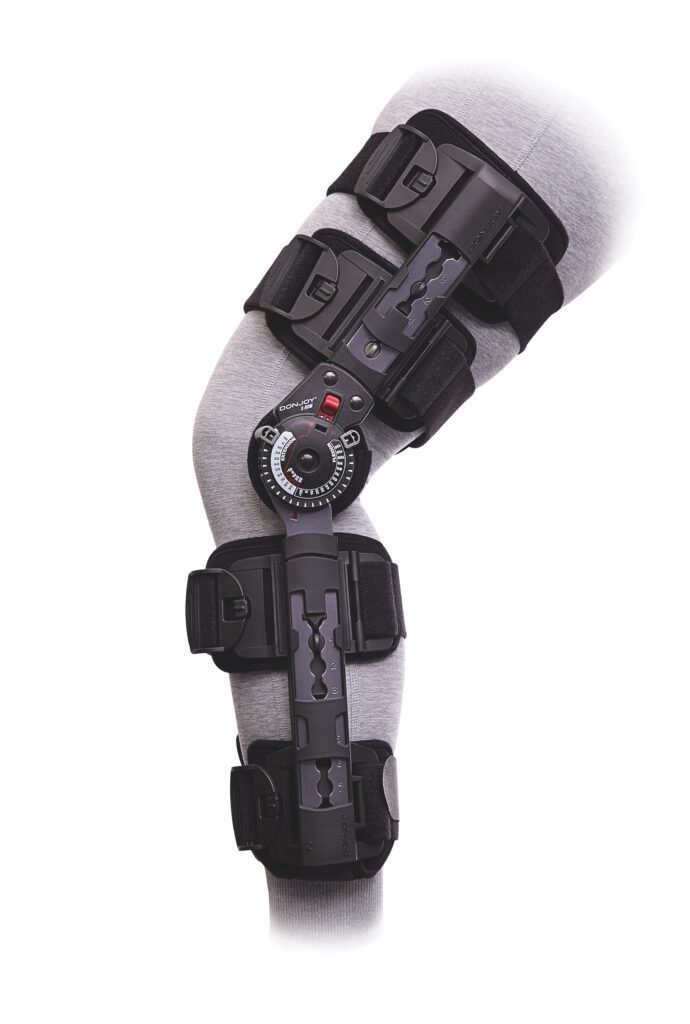
DonJoy® X-ROM™ Post-Op Knee Brace: Early Post-Traumatic and Post-Operative Immobilization
The DonJoy X-ROM™ Post-Op Knee Brace is designed to aid immobilization and provide protected range of motion (ROM) following ACL, PCL, LCL, and MCL surgeries, as well as meniscal repairs. Its updated hinge design allows precise ROM control in 10-degree increments, from -10° to 90° extension and -10° to 120° flexion, with a quick-lock feature for easy setting at a specific angle. Four independently telescoping sliders with push-button control enable rapid, precise fitting across a wide range of patient anatomies. The brace is universal-fit, accommodating patients from 150 cm to 195 cm, and bendable hinge bars allow additional varus or valgus contouring where needed.
For clinicians considering early bracing as part of acute ACL management – whether in the context of the Cross-Bracing Protocol or early post-traumatic immobilization prior to surgery – the X-ROM offers a structured, adjustable platform to deliver controlled immobilization and progressive range of motion as rehabilitation advances.
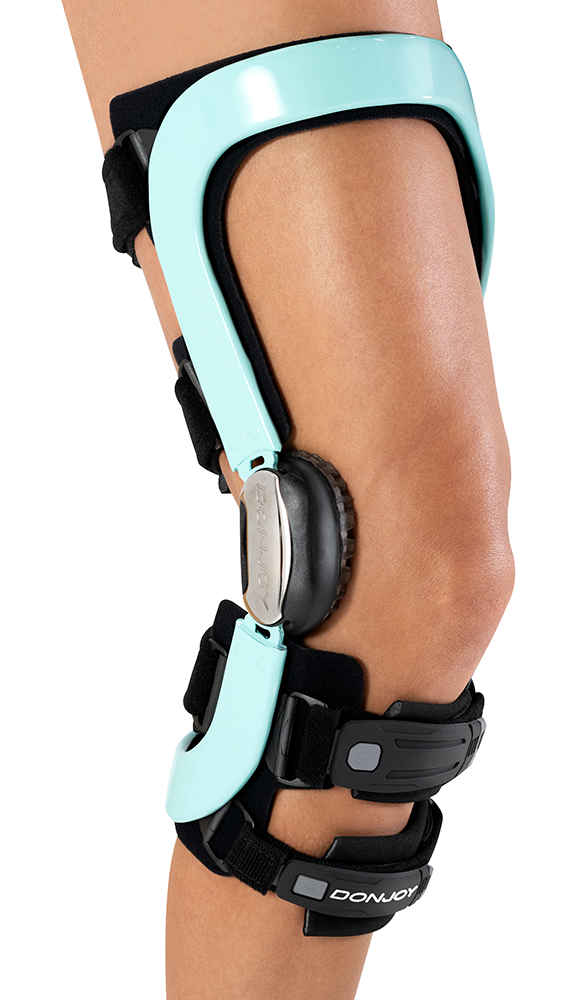
DonJoy® Armor FourcePoint™: Functional Bracing and Return to Sport
The DonJoy Armor FourcePoint™ delivers strong, lightweight protection for moderate to severe ligament instabilities – appropriate for active users and extreme‑sport athletes – combining a moldable aircraft‑grade aluminum frame with the patented Four‑Points‑of‑Leverage™ System and the FourcePoint™ hinge, which dampens knee extension in the high‑risk zone to support stability, reduce re‑injury risk, and ensure a secure, comfortable fit across a wide size range.
A steel-reinforced hinge plate and T6061 aluminum frame deliver robust, lightweight durability suited to contact and extreme sports including football, skiing, snowboarding, and motocross.
For patients who demonstrate favorable healing characteristics on MRI or who are returning to high-demand sport following ACL reconstruction, the Armor FourcePoint provides an evidence-informed, off-the-shelf option to support ongoing knee stability and reduce re-injury risk. Available in seven sizes and two calf lengths, it accommodates bilateral use without impeding performance.
Armor is also available in a version that swaps the FourcePoint hinge for a standard polycentric hinge. By adding flexion stops of (0°), 45°, 60°, 75°, or 90°, or extension stops of 0°, 10°, 20°, 30°, or 40°, this allows incremental flexion-extension ROM control to support different phases of rehabilitation.
For more information on Enovis™ products, visit our website or contact your local Enovis representative.
References
- Filbay SR et al. Healing of acute anterior cruciate ligament rupture on MRI and outcomes following non-surgical management with the Cross Bracing Protocol. Br J Sports Med. 2023 Dec;57(23):1490-1497.
- Filbay SR et al. A new way of grading severity of ACL rupture on acute MRI to consider potential for non-surgical healing with the Cross Bracing Protocol: ACL Acute Rupture Characteristics for Healing (ACL-ARCH) MRI criteria. J Sci Med Sport. 2026 Feb;29(2):145-148.
- Murgier J et al. Does an early post traumatic knee brace reduce the incidence of knee rotational instability? Arch Orthop Trauma Surg. 2024 Mar;144(3):1161-1169.